Contents
Preventing Readmission After Surgery – What Families Often Miss
Coming home after surgery should feel like a victory. In truth, it is the beginning of a fragile phase where every detail matters. Hospitals discharge people once they are stable enough to leave, not fully healed. The first days and weeks at home involve new routines, new medications, physical limitations and emotional stress. That combination makes this period one of the riskiest times for hospital readmission.
The reality is many of these readmissions are avoidable. Families often underestimate the daily challenges of recovery. Meals get skipped or lack protein. Prescriptions pile up and confusion sets in. A trip to the bathroom at night leads to a fall. Appointments are missed because getting to the car is too exhausting. Each gap seems small but together they add up.
At CARE Homecare, we specialize in closing those gaps. As a trusted home care provider in Los Angeles and Orange County, our caregivers support families through this delicate transition. By focusing on daily life; nutrition, mobility, medication reminders, safety and companionship, we reduce the risks that commonly send people back to the hospital.
This article explores the hidden drivers of post-surgical readmissions and how professional home care makes recovery smoother and safer.
Key Takeaways
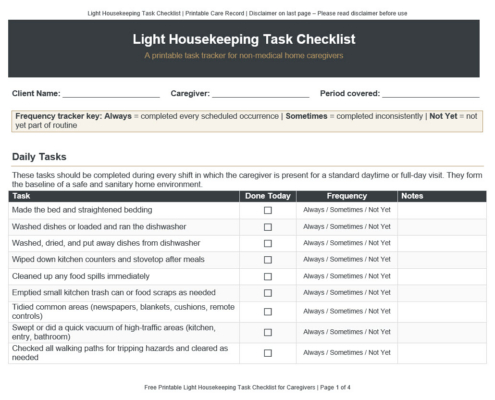
- Many hospital readmissions after surgery are preventable with structure and daily support
- The biggest risks include medication confusion, poor nutrition, falls, unmanaged pain and missed follow ups
- Home care fills the gap between hospital discharge and full independence by supporting daily routines and observing for warning signs
- After hospital discharge, local caregivers in Los Angeles and Orange County add stability, reassurance and logistical support that families cannot always provide alone
- 24 hour home care is a valuable option when overnight safety, toileting or confusion makes families uneasy
Home Care Caregivers in Los Angeles and Orange County
CARE Homecare offers hourly and 24 hour in-home care services across Los Angeles and Orange Counties.
Our caregivers provide trusted support with daily routines, mobility, nutrition, companionship and safety so families can focus on healing instead of worrying.
Readmissions are rarely caused by one issue. They stem from a mix of physical, behavioral and environmental challenges that surface after discharge. Recognizing these risks early is the first step to prevention.
Medication confusion and nonadherence
After surgery, it is common for prescriptions to change. A medication may be added, stopped, or adjusted. Once home, families may find the instructions overwhelming. Pill bottles pile up, timing gets mixed up, or a dose is forgotten. Older adults in particular may slip back into pre-hospital routines.
The CDC reports that adverse drug events send hundreds of thousands of older adults to emergency departments every year, especially during care transitions.
How home care helps: CARE Homecare does not administer or adjust medications, but caregivers provide medication reminders, set up simple pill organizers (supplied by the family or pharmacy) and observe for signs of confusion. If something looks off, like dizziness, constipation or nausea, they alert the family so a licensed clinician can step in quickly. This oversight prevents small issues from spiraling.
Poor nutrition and dehydration
Surgery places heavy demands on the body. Healing requires protein, calories and hydration, yet appetite often drops. Chewing may be uncomfortable. Pain medications can cause nausea or constipation. Fear of eating after abdominal surgery is also common. Without adequate nutrition, wounds heal slowly, strength declines and dehydration increases risk of confusion and kidney stress.
The National Institute on Aging highlights the importance of proper nutrition and hydration for older adults recovering from illness or surgery (NIA Nutrition Guidance).
How home care helps: CARE Homecare caregivers plan and prepare balanced meals tailored to preferences and physician guidance. Protein-rich foods like eggs, yogurt, chicken and fish are prioritized. Soft or blended textures are offered when chewing is difficult. Caregivers also encourage small, frequent meals and regular fluid intake, keeping water or tea within reach throughout the day. By monitoring intake, they notice dips in appetite early and communicate concerns to families.
Falls and mobility setbacks
Limited movement after surgery increases fall risk. Blood pressure may drop when standing, and bulky dressings or new footwear can change balance. Homes are rarely set up like hospital rooms, so throw rugs, tight hallways and poorly lit bathrooms become hazards. Falls within two weeks of discharge are one of the most common reasons people are readmitted.
How home care helps: Our caregivers begin with a room-by-room safety check. Pathways are cleared, throw rugs are removed and lighting is improved. They provide hands-on help with transfers, walking and toileting. CARE Homecare also introduces gentle strengthening routines approved by the family and physician. This combination restores confidence and prevents setbacks.
Pain that is undercontrolled or overcontrolled
Managing pain at home is a delicate balance. Too little pain control discourages movement, leading to stiffness, pneumonia or clots. Too much pain medication increases risk of constipation, drowsiness and falls. Families are often unsure when to encourage the next dose or when to call the doctor.
How home care helps: Caregivers remind clients to take medications as prescribed and observe comfort levels. They encourage non-medication strategies like repositioning, gentle stretches and cold or heat packs when appropriate. If pain appears unmanaged or side effects like confusion or extreme fatigue arise, families are informed promptly.
Missed wound care routines
Incisions need attention to stay clean and heal properly. Dressings may need changing, drains require monitoring and any redness, swelling or unusual drainage should be addressed quickly. Families may feel unsure about whether a wound looks normal or concerning.
How home care helps: CARE Homecare caregivers do not provide wound care, but they remind families of scheduled dressing changes, assist with gathering supplies and encourage hygiene routines like hand washing. Importantly, they observe wounds for visible changes and alert families if something looks unusual so medical providers can intervene promptly.
Skipped follow ups and delayed therapy
Follow-up visits, lab work and therapy sessions are critical for recovery. Yet after surgery, fatigue and mobility challenges make these appointments difficult. Without transportation support, families may cancel or delay care, leading to preventable complications.
How home care helps: CARE Homecare provides transportation assistance so clients can attend follow ups safely. Caregivers help clients prepare for visits, ensure they bring medication lists and encourage questions for the clinician. If in-person visits are too difficult, they support families in arranging telehealth appointments when available.
Sleep disruption and delirium
Sleep is often disrupted in hospitals. Returning home does not always solve the problem, especially when pain, new medications or anxiety interfere. Poor sleep increases fall risk, worsens pain and in older adults may contribute to delirium.
How home care helps: Caregivers establish soothing evening routines, dim lighting and structured sleep-wake schedules. They help with comfort measures like a warm shower, lotion or calming tea. If changes in attention or sudden confusion arise, families are notified immediately.
Confusion about roles
Families often confuse home care with home health care. Home health care involves licensed nurses and therapists who provide wound checks, injections or physical therapy under a doctor’s order. Home care provides non-medical support such as bathing assistance, meal preparation, companionship and supervision. Successful recovery often requires both.
For clarity, you can review Home Care vs Home Health Care and The Differences Between Caregivers, Home Health Aides, Home Care and Home Health Care. CARE Homecare specializes in the daily routines that keep families steady while licensed providers handle the medical tasks.
How CARE Homecare can help prevent costly readmissions
Preventing readmission is about building predictable routines, supporting healthy habits and noticing red flags before they become emergencies. Here’s how a structured home care plan protects recovery.
A clear plan for the first 72 hours
The earliest days after surgery are the most fragile. CARE Homecare helps families implement structured routines that cover medication reminders, hydration, bathroom safety, short supervised walks and rest. For a deeper dive, see our guide on The First 72 Hours at Home After Hospital Discharge.
Daily oversight of medication, meals and movement
Caregivers ensure pill reminders are followed, protein-rich meals are prepared and light exercise is completed safely. Small tasks like keeping water nearby or supervising a bathroom trip make a large difference.
Safe home environment
From light housekeeping to removing hazards, caregivers keep the home organized and clutter-free. Nighttime safety is a priority since many falls happen on the way to the bathroom.
Transportation and appointment support
Whether it is a lab test, follow up with the surgeon or therapy appointment, caregivers provide safe transportation and reduce the stress of logistics.
24 hour support when needed
Some recoveries require continuous oversight, especially when pain or confusion is high. CARE Homecare offers 24 hour home care to provide around-the-clock supervision and reassurance. For families comparing options, see 24 hour care vs live in care.
What success looks like in the first two weeks
A successful two-week recovery at home is calm and predictable. Pain lessens gradually, steps increase day by day, bowels stay regular, the incision remains clean and follow up appointments are completed without crisis. For more detail, see The First Two Weeks at Home After Hospital Discharge – A Practical Playbook.
Families who work with home care providers report reduced anxiety, smoother routines and greater confidence. Clients themselves often feel less isolated, more secure and better able to focus on healing instead of struggling with basic needs.
Evidence-based practices that guide our care
National studies confirm that clear discharge instructions, medication support, nutrition, fall prevention and follow up are the cornerstones of avoiding readmission. The Agency for Healthcare Research and Quality has cataloged proven interventions like early follow up, teach-back education and consistent daily routines.
CARE Homecare aligns with these best practices, translating them into practical steps that families can sustain at home.
Why local care matters in Los Angeles and Orange County
Local challenges like traffic, apartment layouts and busy family schedules add layers of difficulty to recovery. CARE Homecare caregivers know the neighborhoods, resources and best routes, which makes a difference when time and energy are limited. Continuity is also a priority. We strive to provide familiar caregivers so trust grows and anxiety decreases.
If your loved one is preparing to come home after surgery , do not leave recovery to chance. CARE Homecare provides expert non-medical post-surgery home care in Los Angeles or Orange County with planning starting before being discharged from the hospital that reduces risk and supports healing. From meal preparation and medication reminders to mobility support and 24 hour home care, our caregivers in Los Angeles and Orange County help families navigate this critical phase with confidence.
Visit our Contact Us page today to schedule a consultation and build a plan that protects your family from avoidable readmissions.
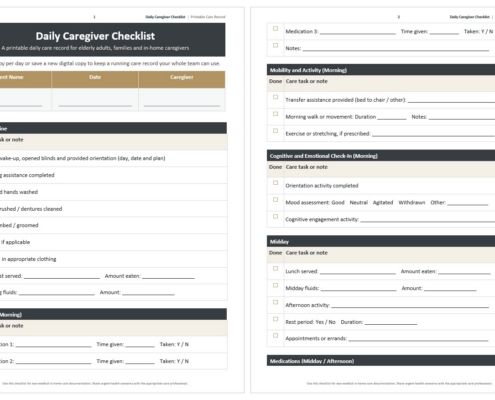
We also put together a free PDF available for download that includes a hospital discharge checklist so your discharge experience is easier and more organized. You can download it here.